Mobile Phone Interventions to Increase Physical Activity and Reduce Weight a Systematic Review
- Research
- Open Access
- Published:
Efficacy of interventions that use apps to amend diet, physical activity and sedentary behaviour: a systematic review
International Journal of Behavioral Nutrition and Concrete Activity volume thirteen, Article number:127 (2016) Cite this article
Abstract
Background
Health and fettle applications (apps) accept gained popularity in interventions to better nutrition, physical activeness and sedentary behaviours but their efficacy is unclear. This systematic review examined the efficacy of interventions that utilize apps to improve diet, physical activeness and sedentary behaviour in children and adults.
Methods
Systematic literature searches were conducted in five databases to identify papers published betwixt 2006 and 2016. Studies were included if they used a smartphone app in an intervention to improve diet, physical activity and/or sedentary behaviour for prevention. Interventions could exist stand up-alone interventions using an app merely, or multi-component interventions including an app as one of several intervention components. Outcomes measured were changes in the health behaviours and related health outcomes (i.east., fitness, body weight, blood pressure, glucose, cholesterol, quality of life). Study inclusion and methodological quality were independently assessed by two reviewers.
Results
20-7 studies were included, most were randomised controlled trials (n = 19; 70%). 20-iii studies targeted adults (17 showed significant health improvements) and four studies targeted children (2 demonstrated meaning wellness improvements). Twenty-i studies targeted physical activity (fourteen showed meaning health improvements), 13 studies targeted diet (seven showed significant wellness improvements) and five studies targeted sedentary behaviour (two showed significant health improvements). More studies (n = 12; 63%) of those reporting significant effects detected between-group improvements in the wellness behaviour or related wellness outcomes, whilst fewer studies (n = 8; 42%) reported significant within-group improvements. A larger proportion of multi-component interventions (8 out of 13; 62%) showed pregnant betwixt-grouping improvements compared to stand-alone app interventions (5 out of 14; 36%). Eleven studies reported app usage statistics, and three of them demonstrated that college app usage was associated with improved health outcomes.
Conclusions
This review provided minor evidence that app-based interventions to improve diet, physical activity and sedentary behaviours can be effective. Multi-component interventions appear to exist more than effective than stand up-alone app interventions, however, this remains to exist confirmed in controlled trials. Future research is needed on the optimal number and combination of app features, behaviour change techniques, and level of participant contact needed to maximise user engagement and intervention efficacy.
Background
The prevention of non-communicable diseases (NCDs) such as cardiovascular disease, cancer and type 2 diabetes is a major public health goal worldwide [1]. In 2012, NCDs were responsible for 38 million (68%) of the globe's 56 1000000 deaths [one]. Lifestyle behaviours including diet, concrete activity and sedentary behaviour are key modifiable take chances factors for these diseases and improving these behaviours is considered essential to reducing the financial and health burden of these NCDs [i]. Unhealthy diet, physical inactivity and sedentary behaviour are known to track from babyhood into adulthood and are difficult to change later on in life [2, 3]. This exacerbates associated health problems and demonstrates why preventing the evolution of these health risk factors throughout the lifespan is important.
Given the global scale of NCDs, preventative interventions that tin reach large populations at low cost are needed. Smartphones and tablets, including the software applications (apps) that run on these devices, take go an integral function of people's life with big increases in usage rates since their introduction in 2007 [4, 5]. For example, 70% of Americans, 61% of Europeans and 74% of Australians regularly use a smartphone and/or tablet [5, 6]. The growth in mobile technologies has also stimulated the growth in health and fitness apps to provide behavioural interventions that can achieve large populations [7]. Clever use of apps in health promotion and prevention of disease has enabled researchers to apply health behaviour changes techniques (e.g., goal setting, self-monitoring, performance feedback) that have proven to facilitate health behaviour change across diverse population groups and settings [7, 8].
Despite the increasing use of apps in health behaviour change studies their efficacy is unclear, particularly for dissimilar lifestyle behaviours such equally diet, physical activity and sedentary behaviour, likewise as for specific population groups including children and adults. Some systematic reviews [9–13] take addressed the potential of health apps to better diet, physical activity and/or sedentary behaviour. Nonetheless, the scope of these reviews has been broad and many questions remain. Firstly, most previous reviews [nine–11, 14] were on electronic and mobile health (east-& mHealth) interventions, not specifically on app-based interventions. Secondly, many reviews [seven, 8, xv–18] have focused on app design, the incorporation of established behaviour change techniques and they examined intervention feasibility rather than efficacy. Thirdly, many previous reviews [19–22] take focused on the use of apps for the treatment of obesity and chronic diseases. Equally such, little is known about the potential of using apps to change wellness behaviours for disease prevention. Finally, no reviews take distinguished between app interventions for children versus adults. This is of import every bit app features highly-seasoned to children and adolescents may differ from those used by adults, and the option of app features will likely determine user engagement, retention and ultimately intervention efficacy [22].
This review aimed to address these gaps in the literature by systematically synthesising evidence for the efficacy of interventions that use apps to improve nutrition, concrete action and sedentary behaviour for NCD prevention. Since app features used by children may differ from those used by adults, we distinguished betwixt app interventions targeted to children and adults.
Methods
Literature search
This review was conducted and reported according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines (Additional file one) [23]. Systematic searches were conducted between November and December 2015 in five databases: Scopus, CINAHL, SportDiscuss, PsycINFO and Web of Science. The search was express to English language literature, humans, and the year of publication betwixt 01 January 2006 and 31 October 2016. It was considered unlikely that app interventions were developed before 2006/2007 when smartphones were introduced. Systematic search strategies were designed using a combination of thesaurus and costless terms covering the following terms: application, app, smartphone, smart phone, tablet, mobile game, game, physical activity, walk, concrete fitness, leisure activeness, motor activeness, exercise, sport, sedentary, sedentary behaviour, sedentary behavior, sitting, screen time, inactive, nutrition, dietary, nutrition, nutritional, salubrious eating, nutrient, fruit, vegetable, snack, soft beverage, carbonated drink, intervention, programme, programme, health promotion, prevention and trial. The detailed search strategies used for each database are presented in the Boosted file 2. Additionally, articles were identified via hand-searching and reviewing reference lists of relevant papers.
Inclusion criteria and report pick
Studies were included in the present review if (1) they used an app in an intervention to influence at least i of the following lifestyle behaviours: dietary intake, concrete activity, sedentary behaviour; (2) targeted children and/or adults; (three) focused on behaviour alter for affliction prevention (i.e., not specifically aiming to treat and manage health conditions such every bit obesity, hypertension and NCDs); and (four) reported information regarding efficacy for behaviour change (e.g., change in daily minutes of physical action). In addition, studies could too report (just were not required) other relevant outcomes that may have feasibly been impacted by wellness behaviour change (i.eastward., fettle, body weight, blood pressure, glucose, cholesterol, quality of life). All types and units of measurements for the lifestyle behaviours and related wellness outcomes were acceptable (e.m., objective measure out, cocky-study, minutes, steps, servings, calories, kilograms). The app intervention could be a stand-lonely intervention using apps simply, or a multi-component intervention where the employ of an app was one of several intervention components (e.k., physical education, provision of physical action equipment, parental education, face up-to-face counselling). Studies were excluded from the review if: (1) non-experimental study designs were utilised (i.east., observational or case studies, studies reporting prevalence or trend data, feasibility studies, measurement studies, theoretical papers); and (ii) the publication was non a peer-reviewed primary study (i.eastward., letters, commentaries, briefing proceedings, reviews, narrative articles). Initially, titles and abstracts were screened for inclusion by a single reviewer (SS). Equally per best exercise for systematic reviews [23], two reviewers (SA, WVL) independently reviewed the eligibility of studies for inclusion in the review, with disagreement resolved past discussion and consensus with a third reviewer (SS).
Data extraction
Data extraction was conducted using a standardised form developed specifically for this review (Table one); similar to those used in other systematic reviews [12, 24, 25]. For all included studies, data were extracted for author, year, state, study design, intervention duration, measurement time points, attrition rate, sample, behaviour modify theory, app features including behaviour modify techniques, intervention components, outcomes, measures and main study results. The primary issue measures extracted for main study results were dietary intake, concrete activity and sedentary behaviour. Other relevant outcome measures closely related to these behaviours included weight condition (body mass index, trunk weight, waist circumference), fitness, blood pressure, cholesterol, glucose and quality of life. To determine whether the interventions had a significant effect on behavioural and wellness outcomes, information on significance and magnitude of within- and between-grouping differences was extracted. For each included report, two reviewers independently extracted information (NAB and either SS, SA or WVL). Reviewers one and ii agreed on the data extraction in over 70% of the studies. Disagreement was hands resolved past discussion and consensus with a tertiary reviewer (either SS, SA or WVL).
Study quality cess
The quality of the included studies was assessed using 25-point criteria adapted from the Espoused checklists for the reporting of randomised controlled trials [26]. While the CONSORT checklist is intended for controlled trials, most criteria are applicative to other study designs and the weaker study designs justifiably received a lower score than studies using a controlled trial pattern. This approach has been used in other reviews [24]. Each criterion was rated as one (fulfilled), 0.5 (non all sub-items making up the criterion were fulfilled), 0 (not fulfilled or unclear), or not applicable (criterion was not applicable to the written report blueprint). Non applicable criteria were discounted from the 'overall study quality score' (sum of points). Hence, the highest attainable quality score was not 25 for all studies. Adjusted from previous reviews [27, 28], the obtained study quality score for each study was divided by the highest attainable score and multiplied by 100 to give a percentage of fulfilled criteria; and studies were then grouped into loftier (>66.7%), off-white (fifty–66.6%) or low (<50%) study quality (Additional file 3). The study quality cess was conducted independently by two reviewers (SS, SA), with disagreement resolved past give-and-take and consensus with a tertiary reviewer (WVL). Percent agreement between reviewers one and two for the scoring of the CONSORT criteria was 89%, with the most common points of discrepancy relating to recruitment methods, outcomes reporting and blinding procedures.
Results
Study choice
A flowchart of the study selection process is presented in Fig. 1. A total of 6926 publications were identified from the database search. Afterward removal of duplicates, 4945 publication titles and abstracts were screened, and 194 total-text manufactures were considered potentially eligible for inclusion. Of these, 30 articles reporting information on the efficacy of an app-based intervention to amend nutrition, physical activity and/or sedentary behaviour for prevention were included for last review. Some articles [29–34] reported on the same studies, and as such, a total of xxx articles describing 27 studies were included in this review.
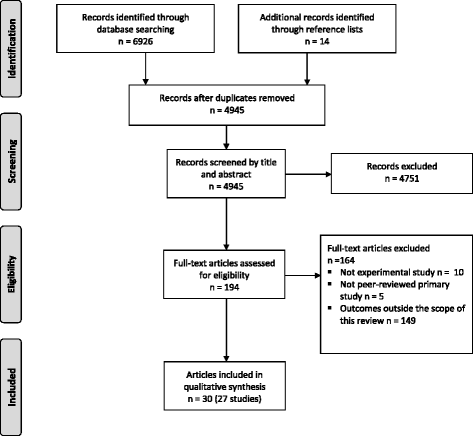
Flowchart of study choice procedure
Written report characteristics
Characteristics of the app intervention studies included in this review are presented in Tabular array i.
Twelve studies were conducted in Due north America [35–46], seven studies in Australia/New Zealand [29–32, 47–51], seven studies in Europe [33, 34, 52–57], and one study in the Middle-Eastward [58]. Most studies were randomised controlled trials (northward = 19) with two-grouping [29, 31, 35, forty, 43–46, 48, fifty, 52–55, 58] or 3-group [33, 34, 42, 47, 56, 57] study designs. The remaining studies were controlled trials (n = 3) [33, 37, 49], randomised trials (due north = 1) [39] or pre-post studies (n = 4) [36, 38, 41]. Twenty-three studies [31–36, 38, 39, 41–46, 48–58] targeted adults (mean age: 41.5 years, range: xviii–71 years) and four studies [29, 37, 40, 47] targeted children or adolescents (mean historic period: 12.iv years, range: eight–17 years). The total number of participants beyond the 27 studies was 2699 (510 children/adolescents, 2189 adults). Samples sizes ranged from 17 to 502 (mean sample size: 100). The duration of interventions ranged from ane–24 weeks, with an average intervention duration of ten weeks. Follow-up assessments were at 4 weeks (n = 5), 8 weeks (due north = 8), 12 weeks (n = nine), 20 weeks (n = two), half dozen months (n = 2), ix months (north = i) and 18 months (n = 1). Attrition rates ranged from 0% [36] to 57% [51], with an boilerplate attrition rate of 17%. The majority of studies [31, 33, 35–45, 47, 48, fifty, 53, 55–58] reported higher rates of female person participation (on boilerplate 64% of participants were female person). The targeted health behaviours were dietary intake (north = 13), concrete activity (n = 21) and sedentary behaviour (due north = 5). Other reported lifestyle-related health outcomes were: weight status (n = 11); fitness (n = iii); blood pressure (north = 4); blood glucose (n = 1); cholesterol (n = 1); and quality of life (n = 2). Ten studies [33, 36–38, 43–45, 49, 50, 55, 57] targeted a single health behaviour, whilst 17 studies [29, 31, 35, 39–42, 46–48, 50–56, 58] targeted multiple wellness behaviours and related health outcomes. Fourteen studies [33, 37–twoscore, 42, 45–47, 51, 52, 55–57] involved interventions delivered solely via an app (stand-solitary intervention) and thirteen studies [29, 31, 35, 36, 41, 43, 44, 48–fifty, 53, 54, 58] involved interventions that used apps in conjunction with other intervention strategies (multi-component intervention), such as concrete didactics, parental education, counselling sessions, printed materials, motivational emails, websites and pedometer employ. Fifteen studies [29, 31, 36–39, 45, 46, 48–50, 52, 56–58] used a newly designed app in the intervention and 12 studies [33, 35, 40–44, 47, 51, 53–55] used a commercially available app. Further, 15 of the 27 studies reported intervention designs based on behaviour alter theories, such as Cocky-determination Theory (n = 3) [29, 35, 37], Transtheoretical Model (n = 4) [31, 33, 41, 48], Social Cerebral Theory (n = four) [29, 39, 44, 46], Theory of Planned Behaviour (n = 2) [45, l], Command Systems Theory of Self-regulation (north = ane) [58], and the Behaviour Change Wheel (north = one) [55].
Study quality
A detailed summary of quality assessments of included studies is presented in the Additional file iii. Overall, study quality ranged from high (north = 11) [29, 31, 43–45, 47, 48, l, 53, 54, 58], to off-white (n = eight) [35, 37, 46, 49, 55–57], and low (north = 8) [33, 36, 38, 39, 41, 42, 51, 52]. Study quality of interventions targeted to children/adolescents was high (n = 2) [29, 47] and fair (northward = two) [37, 40], and study quality of interventions targeted to adults ranged from high (n = 9) [31, 44, 45, 48, 50, 53, 54, 58], to fair (due north = half-dozen) [35, 46, 49, 55–57], and low (n = viii) [33, 36, 38, 39, 41, 42, 51, 52]. Well-nigh of the 13 interventions that used an app in combination with other intervention strategies were of loftier quality (n = 9) [29, 31, 43, 44, 48, fifty, 53, 54, 58], whilst well-nigh of the 14 stand up-alone app interventions were of off-white (n = six) [37, forty, 46, 55–57] or low quality (n = 6) [33, 38, 39, 42, 51, 52]. Study quality did not differ markedly between app interventions targeting multiple health behaviours and related wellness outcomes (high: n = viii, fair: n = four, depression: n = 5) and those targeting a unmarried health behaviour (loftier: northward = iii, fair: n = iv, depression: northward = 3). On average, the included studies fulfilled 61% of the cess criteria (range: 34–92%). Almost studies met the Consort requirements to provide a strong scientific rationale and described their participant eligibility, statistical methods and interventions conspicuously. Fewer studies reported sample size calculations [29, 31, 35, 43, 47, l, 53–55, 57, 58] and included randomisation [29, 31, 35, 37, 39, 43–48, 50, 52–55, 58] and blinding procedures [31, 44–50, 53] in their study pattern. Attrition rates were reported or could exist calculated for the majority of studies [29, 31, 33, 35–51, 53–58].
Intervention efficacy
A summary of intervention effects for the included lifestyle behaviour outcomes (diet, physical activity, sedentary behaviour) and related wellness outcomes (weight status, fitness, claret pressure, glucose, cholesterol, quality of life) are presented in Tabular array 2. Overall, a slightly larger proportion of single health behaviour interventions (5 out of 10; 50%) [33, 45, 49, 55, 57] showed meaning between-group improvements than multiple health behaviour interventions (seven out of 17; 41%) [29, 31, 48, 50, 53, 54, 58]. Further, a larger proportion of interventions that used an app in conjunction with other intervention strategies (8 out of 13; 62%) demonstrated significant betwixt-group improvements in the behavioural and health outcomes [29, 31, 48–50, 53, 54, 58] compared to stand-alone app interventions (5 out of 14; 36%) [33, 40, 45, 55, 57].
Children and adolescents
Of the four studies that specifically targeted children and/or adolescents, i study [29] reported significant between-group improvements in nutrition, sedentary behaviour and fitness in the app intervention group. Another study [37] reported a significant within-group increase in concrete activity, but no meaning departure between groups. The remaining two studies [40, 47] reported no pregnant changes in the behavioural or related health outcomes.
Adults
Of the 23 studies that targeted adults, 17 studies reported significant improvements in diet (n = 6) [31, 38, 45, 54, 57, 58], concrete activity (n = 13) [31, 33, 36, 37, 39, 41, 43, 48–50, 53–55, 58], sedentary behaviour (n = 1) [39], and other improved outcomes including weight status (north = 4) [31, 41, 42, 58], 49], fitness (north = 1) [56], blood force per unit area (n = two) [41, 56] and cholesterol (n = 1) [41]. Of the studies reporting pregnant findings, 11 studies detected significant between-grouping differences in diet (n = 5) [31, 45, 54, 57, 58], physical action (due north = nine) [31, 33, 48–l, 53–55, 58] and weight status (northward = ii) [31, 58] in favour of the app intervention group. Seven studies institute significant inside-group improvements in diet (due north = one) [38], physical action (n = iv) [33, 36, 37, 39, 41, 43], sedentary behaviour (n = 1) [39] and weight condition (northward = 2) [41, 42, 56], blood pressure (north = 2) [41, 56] and cholesterol levels (n = 1) [41]. Five studies [35, 44, 46, 51, 52] reported no significant changes in the health outcomes of interest, and no significant findings were found in relation to the outcome glucose levels (assessed in one study).
Characteristics of efficacious interventions
App interventions showing significant between-group improvements in the behavioural and health outcomes tended to exist multi-component interventions [31, 36, 41, 43, 48–50, 53, 54, 58], with sample sizes higher up ninety participants [35, 43, 44, 47–49, 53] and intervention durations longer than 8 weeks [37, 42–45, 47, 49]. A slightly larger proportion of single health behaviour [33, 45, 49, 55, 57] versus multiple health behaviour interventions [29, 31, 48, 50, 53, 54, 58] demonstrated between-group improvements (fifty% versus 41%, respectively). Farther, most of the interventions [29, 31, 33, 39, 42, 45, 48–l, 53, 55, 56, 58] showing significant improvements in the behavioural and health outcomes included goal-setting, self-monitoring and performance feedback in the app blueprint. Some efficacious interventions also incorporated other behaviour change techniques, such every bit motivational messages [29, 36, 57], health educational activity/tailored communication [29, 31, 38, 48, 54, 57], reinforcement [33, 39, forty, 45], gamification in the form of exergames, award and rewards [37–40, fifty], social support through interaction with peers [33, 37, 50] and friendly team challenges [29, 37, 39, 45]. There was not plenty data to identify which behaviour change techniques adamant intervention efficacy. Moreover, there was no difference in the behaviour change techniques incorporated in apps for children compared to those used in apps for adults. 11 studies [31, 38, 40, 43, 45, 48–fifty, 54, 56–58] out of the 19 studies showing pregnant improvements in behavioural and wellness outcomes reported usage statistics to make up one's mind participants' date with the app. Three of these studies [38, 43, 49] examined associations betwixt app usage and changes in the behavioural and wellness outcomes. Their findings showed that college app usage was associated with improvements in physical activity and healthy eating [38, 43, 49].
Discussion
This systematic review found modest testify for the efficacy of app interventions to improve nutrition, physical activeness and sedentary behaviours for NCD prevention. Overall, 19 out of the 27 identified studies reported significant improvements in behavioural and related wellness outcomes. Most of these studies reported significant betwixt-group improvements in the app intervention group versus comparing grouping, which is considered the gold standard to demonstrate intervention efficacy [59]. Yet study limitations, the findings from this review indicate that apps can exist an effective tool to improve health behaviours. The advantages of smartphone apps over other intervention delivery modes such as websites, face-to-face counselling and group sessions may partially explain the efficacy of app interventions. Given that many people have busy lifestyles, they value convenient admission to health behaviour modify programs that provide data and advice, real-fourth dimension self-monitoring, feedback, reinforcement, social support, and rewards 'on the become' [threescore]. The entreatment of smartphones for help in wellness promotion concurs with the trend that more than people are seeking health information via mobile devices [61, 62]. In this context, apps provide the opportunity to bring behavioural interventions into existent life situations where people make decisions about their health.
Despite the potential of apps, one-half of the interventions identified in this review used apps in conjunction with other intervention strategies. The remaining interventions were stand-lone interventions where the app was the sole intervention component. Chiefly, yet, is the observation that most of the multi-component interventions demonstrated significant between-grouping improvements in behavioural and wellness outcomes, whereas fewer stand up-lonely app interventions reported significant between-group improvements. This raises the question whether multi-component interventions yield stronger intervention furnishings than stand-solitary app interventions. Many reviews of health behaviour alter interventions [63–67] recommend the apply of multiple intervention strategies to achieve long-term health behaviour change. Reviews of website-delivered interventions [nine, 28, 68] have also shown stronger behaviour alter furnishings when combined with other intervention strategies such equally SMS, telephone coaching and motivational emails. Every bit such, information technology is likely that the integration of apps in multi-component interventions produces stronger wellness outcomes compared to stand-alone app interventions; nevertheless, this remains to be tested in hereafter trials.
The majority of app interventions were targeted to adults; merely four out of the 27 identified app interventions were specifically aimed at children or adolescents. This is consistent with previous eastward & mHealth reviews [11, 12, 25, 69] showing that internet and mobile phone delivered interventions have mainly targeted adult populations. Although smartphones and tablets have become an integral part of children'due south lives [70], surprisingly few interventions have notwithstanding utilised app technology in pediatric wellness behaviour alter programs [12]. Yet, every bit exergame and serious game apps are becoming increasingly popular among children and adolescents [71], it is probable that more app studies focussing on children will be conducted in the near future.
The average attrition rate (i.e., participant loss to follow-up) reported in the app interventions was 17%, which is lower compared boilerplate attrition rates of 23–27% found in web-based interventions [28, 68, 72]. Lower participant attrition indicates less bias in the estimated intervention furnishings [73]. However, participant compunction does not capture participants' date with the app intervention which also determines intervention effects. For example, web- and app-based interventions that take examined participant date found that higher levels of website and app usage were associated with increased intervention efficacy [38, 43, 68]. Despite this, less than half of the studies reported usage statistics to determine participants' engagement with the app. This is consistent with previous reviews [24, 28, 68] reporting that few internet and mobile interventions recorded participants' appointment with the intervention technologies. Given the relative ease by which app usage statistics can be tracked, it is unfortunate that this information is non existence nerveless and published for all studies in this area. We know that participant date, measured by number of website logins, usually declines later on the outset few weeks in website and social media interventions [24, 28, 68]. An example is the Australian x,000 Steps program, a successful, freely bachelor web- and app-based intervention to promote physical activity [61]. Participants' engagement with the 10,000 Steps website and app lasts on average 5–6 weeks, with longer usage duration (on average 8 weeks) being observed in people who utilize both the 10,000 Steps website and app [61]. This rapid reject in usage concurs with qualitative inquiry showing that people often lack delivery to using whatever item app and they tend to appoint in but transient, casual app use [sixty]. Since participant date determines intervention exposure, and level of intervention exposure determines intervention efficacy [28, 61, 74], improve understanding of factors that improve participant engagement and retention is needed.
To increase user engagement with health behaviour change apps, more information is needed about what app features and behaviour alter techniques people value and apply. Recent focus group information showed that [lx, 75] that young people value health behaviour apps that require depression try, are pleasant to use, are developed by credential experts, enable self-monitoring, provide advice on how to alter behaviour, include positively framed alerts/reminders (merely non too frequent), provide accurate tracking functions, incorporate adequate privacy settings, and clearly bear witness what the app will practice (no surprises). Some of these user preferences were role of the efficacious apps identified in this review. For example, most apps included goal-setting, self-monitoring and performance feedback [29, 31, 33, 39, 42, 45, 48–50, 53, 55, 56, 58]. Additionally, some apps incorporated tailored advice, motivational prompts and reinforcement, gamification, social back up or friendly team challenges [29, 33, 37–twoscore, 45, 48, 50, 54, 57]. Reviews of spider web-based interventions have demonstrated that interventions including more behaviour alter techniques are more than effective [74, 76]. This may also utilize to app-based interventions. However, it remains unclear what the optimal number and combination of app features and behaviour modify techniques is to increase user retention and ultimately intervention efficacy. It is also possible that efficacy declines when too many features or techniques are implemented. Furthermore, socio-demographic factors (e.yard., sex, age, teaching) and psychosocial factors (e.g., attitudes, perceived benefits, enjoyment) may as well influence app usage [threescore]. Emerging research on the adoption of app technology showed that higher app usage is associated with being female and of younger age [61, 77], as well every bit with personal interest in new technologies, positive attitudes towards smartphone apps and perceived benefit of employ [77]. Therefore, targeting and tailoring smartphones apps to specific population groups may besides raise the efficacy of app-based interventions.
Strengths and limitations
Strengths of this systematic review are that it was conducted and reported according to PRISMA guidelines [23], and study quality was systematically assessed using the Espoused checklist [26]. The search strategy was comprehensive, and study pick, information extraction, and quality rating were completed past ii contained reviewers, as is standard practice for loftier quality systematic review [23]. These procedures ensure accurateness of the reviewed information. The telescopic of this review was express to app interventions improving behavioural and related health outcomes for prevention; hence app interventions relating to chronic disease treatment were not captured in this review. Few app interventions identified in this review focused on dietary and sedentary behaviours which makes it more hard to describe conclusions on the efficacy of app interventions targeting these behaviours, as opposed to those targeting concrete activity behaviour. Furthermore, the included studies varied widely in terms of methodological quality, with some studies scoring very poorly, thereby reducing the trust that can be placed in their findings. Finally, the possibility of publication bias should besides be acknowledged. Every bit with all systematic reviews examining the efficacy of interventions, it is possible that some studies with null findings accept non been published [78].
Recommendations for future enquiry
Based on this review, it is recommended that futurity studies:
-
Test the efficacy of specific app features and behaviour modify techniques in high quality controlled trials to distinguish effective from ineffective intervention components.
-
Directly compare the efficacy of stand-alone app intervention compared to multi-component interventions that use apps in combination with other intervention strategies.
-
Compare the efficacy of app interventions to other intervention delivery modes, such as website, print-based and face up-to-face interventions.
-
Utilise larger sample sizes to ensure they are sufficiently powered to discover significant intervention furnishings.
-
Tailor app interventions to specific population groups (e.chiliad., women, young people) in whom usage and adoption of app technology is high.
-
Report app usage statistics using objective and self-study measures to examine levels of and reasons for participant (dis)engagement and intervention exposure.
-
Explore the optimal duration and intensity of app interventions to ensure user engagement and memory equally the intervention progresses.
-
Identify factors that increase user engagement and retention in app interventions to sustain behavioural health improvments in the long-term.
-
Investigate the relationship between user engagement and intervention efficacy, whilst taking into business relationship socio-demographic and psychosocial factors.
Conclusions
Interventions using apps to better diet, physical activity and sedentary behaviour for prevention evidence promise for effective behaviour change in children and adults. The bear witness base of operations is largest for the utilise of apps to increase concrete activity in adults. Fewer interventions have used apps to improve dietary and sedentary behaviours, and very few app interventions take targeted children and adolescents. Multi-component interventions that combine apps with other intervention strategies appear to be more effective than stand up-alone app interventions, however, this remains to be tested further in controlled trials. Overall, in that location is even so considerable telescopic to improve the efficacy of app-based interventions. In particular, intervention studies should gather more app usage statistics to identify factors that meliorate user engagement and retention, and its relationship with intervention efficacy. In addition, more determinative research is needed to determine the optimal number and combination of app features, behaviour alter techniques, and level of participant contact needed to maximise user engagement and ultimately intervention efficacy.
Abbreviations
- Apps:
-
Applications
- Consort:
-
Consolidated standards of reporting trials
- NCDs:
-
Non-catching diseases
- PRISMA:
-
Preferred reporting items for systematic reviews and meta-analyses
References
-
World Health Organization. Global status study on noncommunicable diseases. World Health Organization. 2014. http://world wide web.who.int/nmh/publications/ncd-status-report-2014/en/. Accessed 5 Jul 2016.
-
Biddle SJ, Pearson N, Ross GM, Braithwaite R. Tracking of sedentary behaviours of immature people: a systematic review. Prev Med. 2010;51:345–51.
-
Craigie AM, Lake AA, Kelly SA, Adamson AJ, Mathers JC. Tracking of obesity-related behaviours from childhood to adulthood: a systematic review. Maturitas. 2011;seventy:266–84.
-
Statistica. Number of smartphone users worldwide from 2014 to 2019. Statistica. 2016. http://www.statista.com/statistics/330695/number-of-smartphone-users-worldwide/. Accessed v Jul 2016.
-
Australian Communications and Media Authority. Communications written report 2014–15. Australian communications and media authorisation. 2015. http://www.acma.gov.au/theACMA/Library/Corporate-library/Corporate-publications/communications-study-2014-15. Accessed 5 July 2016.
-
Grouping Special Mobile Clan. The mobile economy. Grouping special mobile clan. 2015. http://www.gsmamobileeconomy.com/GSMA_Global_Mobile_Economy_Report_2015.pdf. Accessed v July 2016.
-
Middelweerd A, Mollee JS, van der Wal CN, Brug J, te Velde SJ. Apps to promote physical activity among adults: a review and content analysis. Int J Behav Nutr Phys Deed. 2014;11:97.
-
Direito A, Pfaeffli Dale 50, Shields Eastward, Dobson R, Whittaker R, Maddison R. Do concrete activity and dietary smartphone applications incorporate prove-based behaviour alter techniques? BMC Public Wellness. 2014;fourteen:646.
-
Hutchesson MJ, Rollo ME, Callister R, Collins CE. Cocky-monitoring of dietary intake by young women: Online food records completed on estimator or smartphone are every bit accurate as paper-based nutrient records but more adequate. J Acad Nutr Diet. 2015;115:87–94.
-
Fanning J, Mullen SP, McAuley Due east. Increasing physical action with mobile devices: a meta-analysis. J Med Cyberspace Res. 2012;14:61–71.
-
Monroe CM, Thompson DL, Bassett DR, Fitzhugh EC, Raynor HA. Usability of mobile phones in physical action–related inquiry: a systematic review. Am J Wellness Educ. 2015;46:196–206.
-
Bort-Roig J, Gilson ND, Puig-Ribera A, Contreras RS, Trost SG. Measuring and influencing physical activity with smartphone technology: a systematic review. Sports Med. 2014;44:671–86.
-
Zhao J, Freeman B, Li 1000. Tin mobile phone apps influence people'southward wellness behavior alter? An evidence review. J Med Internet Res. 2016;18:e287.
-
Lau Pow, Lau EY, Wong del P, Ransdell Fifty. A systematic review of information and advice technology-based interventions for promoting concrete activity behavior alter in children and adolescents. J Med Internet Res. 2011;13:e48.
-
Schoffman DE, Turner-McGrievy G, Jones SJ, Wilcox Southward. Mobile apps for pediatric obesity prevention and treatment, salubrious eating, and concrete action promotion: Just fun and games? Transl Behav Med. 2016;3:320–five.
-
Conroy DE, Yang CH, Maher JP. Behavior change techniques in top-ranked mobile apps for physical activity. Am J Prev Med. 2014;46:649–52.
-
Sharp DB, Allman-Farinelli M. Feasibility and validity of mobile phones to assess dietary intake. Nutr. 2014;30:1257–66.
-
Payne HE, Lister C, West JH, Bernhardt JM. Behavioral functionality of mobile apps in health interventions: a systematic review of the literature. JMIR Mhealth Uhealth. 2015;three:e20.
-
Wang J, Wang Y, Wei C, Yao NA, Yuan A, Shan Y, et al. Smartphone interventions for long-term health management of chronic diseases: an integrative review. Telemed J Due east Health. 2014;xx:570–83.
-
Woo J, Chen J, Ghanavati Five, Lam R, Mundy N, Li LC. Effectiveness of cellular phone-based interventions for weight loss in overweight and obese adults: a systematic review. Orthop Muscul Syst. 2013;3:141.
-
Okorodudu DE, Bosworth HB, Corsino L. Innovative interventions to promote behavioral change in overweight or obese individuals: a review of the literature. Ann Med. 2015;47:179–85.
-
Bardus Thou, van Beurden SB, Smith JR, Abraham C. A review and content analysis of engagement, functionality, aesthetics, information quality, and alter techniques in the near popular commercial apps for weight management. Int J Behav Nutr Phys Act. 2016;xiii:35.
-
Moher D, Liberati A, Tetzlaff J, Altman DG, Group TP. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6:e1000097.
-
Maher CA, Lewis LK, Ferrar Yard, Marshall Due south, De Bourdeaudhuij I, Vandelanotte C. Are health beliefs change interventions that employ online social networks effective? A systematic review JMIR. 2014;16:e40.
-
Stephens J, Allen J. Mobile telephone interventions to increase concrete activity and reduce weight: a systematic review. J Cardiovasc Nurs. 2013;28:320–nine.
-
Moher D, Hopewell Due south, Schulz KF, Montori V, Gøtzsche PC, Deveraux PJ, et al. CONSORT 2010 explanation and elaboration: updated guidelines for reporting parallel group randomised trials. BMJ. 2010;340:c869.
-
Schoeppe S, Duncan MJ, Badland H, Oliver M, Curtis C. Associations of children'southward independent mobility and agile travel with concrete activeness, sedentary behaviour and weight status: a systematic review. JSAMS. 2013;16:312–nine.
-
Davies C, Spence JC, Vandelanotte C, Caperchione CM, Mummery WK. Meta-analysis of internet-delivered interventions to increment physical activity levels. Int J Behav Nutr Physl Deed. 2012;9:52.
-
Smith JJ, Morgan PJ, Plotnikoff RC, Dally KA, Salmon J, et al. Smart-phone obesity prevention trial for boyish boys in low-income communities: the ATLAS RCT. Pediatrics. 2014;134:e723–31.
-
Lubans DR, Smith JJ, Plotnikoff RC, Dally KA, Okely Advertising, Salmon J, et al. Assessing the sustained impact of a school-based obesity prevention program for adolescent boys: the ATLAS cluster randomized controlled trial. Int J Behav NutrPhys Act. 2016;thirteen:92.
-
Partridge SR, McGeechan Thou, Hebden L, Balestracci K, Wong ATY, Denney-Wilson East, et al. Effectiveness of a mHealth lifestyle programme with phone support (TXT2BFiT) to forestall unhealthy weight gain in young adults: randomized controlled trial. JMIR Mhealth Uhealth. 2015;3:e66.
-
Allman-Farinelli One thousand, Partridge SR, McGeechan K, Balestracci K, Hebden L, Wong A, et al. A mobile health lifestyle program for prevention of weight gain in young adults (TXT2BFiT): Nine-month outcomes of a randomized controlled trial. JMIR Mhealth Uhealth. 2016;4:e78.
-
Silveira P, van de Langenberg R, van het Reve E, Daniel F, Casati F, de Bruin ED. Tablet-based strength-residual preparation to motivate and improve adherence to exercise in independently living older people: a stage II preclinical exploratory trial. JMIR. 2013;15:114–xxx.
-
van het Reve East, Silveira P, Daniel F, Casati F, de Bruin ED. Tablet-based forcefulness-residue training to motivate and better adherence to do in independently living older people: function 2 of a phase Ii preclinical exploratory trial. JMIR. 2014;16:99–116.
-
Cowdery J, Majeske P, Frank R, Brown D. Exergame apps and physical activity: the results of the ZOMBIE trial. Am J Health Educ. 2015;46:216–22.
-
Fukuoka Y, Vittinghoff Due east, Jong SS, Haskell Westward. Innovation to motivation: Pilot study of a mobile telephone intervention to increment physical activeness among sedentary women. Prev Med. 2010;51:287–9.
-
Garde A, Umedaly A, Abulnaga SM, Robertson L, Junker A, Chanoine JP, et al. Assessment of a mobile game ('MobileKids Monster Manor') to promote physical activeness among children. Games Health. 2015;4:145–viii.
-
Gilliland J, Sadler R, Clark A, O'Connor C, Milczarek M, Doherty Due south. Using a smartphone application to promote salubrious dietary behaviours and local nutrient consumption. Biomed Res Int. 2015. doi:10.1155/2015/841368.
-
Rex Air conditioning, Hekler EB, Grieco LA, Winter SJ, Sheats JL, Buman MP, et al. Harnessing unlike motivational frames via mobile phones to promote daily physical activity and reduce sedentary behavior in aging adults. Plos One. 2013;8:e62613.
-
Nollen NL, Mayo MS, Carlson SE, Rapoff MA, Goggin KJ, Ellerbeck EF. Mobile engineering science for obesity prevention: a randomized airplane pilot study in racial- and ethnic-minority girls. Am J Prev Med. 2014;46:404–eight.
-
Stuckey M, Russell-Minda Due east, Read Due east, Munoz C, Shoemaker K, Kleinstiver P, et al. Diabetes and technology for increased activity (Information) study: results of a remote monitoring intervention for prevention of metabolic syndrome. J Diabetes Sci Technol. 2011;5:928–35.
-
Wharton CM, Johnston CS, Cunningham BK, Sterner D. Dietary self-monitoring, but not dietary quality, improves with employ of smartphone app applied science in an 8-calendar week weight loss trial. J Nutr Educ Behav. 2014;46:440–four.
-
Wang JB, Cadmus-Bertram LA, Natarajan L, White MM, Madanat H, Nichols JF, et al. Clothing sensor/device (Fitbit One) and SMS text-messaging prompts to increment physical activity in overweight and obese adults: a randomized controlled trial. Telemed J Due east Health. 2015;21:782–92.
-
Choi JW, Lee J, Vittinghoff E, Fukuoka Y. mHealth concrete activity intervention: a randomized airplane pilot study in physically inactive pregnant women. Matern Child Health. 2016;20:1091–101.
-
Mummah SA, Mathur M, King Air conditioning, Gardner CD, Sutton S. Mobile technology for vegetable consumption: a randomized controlled pilot study in overweight adults. JMIR Mhealth Uhealth. 2016;4:e51.
-
Rabbi M, Pfammatter A, Zhang M, Spring B, Choudhury T. Automated personalized feedback for physical action and dietary behavior change with mobile phones: a randomized controlled trial on adults. JMIR Mhealth Uhealth. 2015;iii:e42.
-
Direito A, Jiang Y, Whittaker R, Maddison R. Apps for IMproving Fettle and increasing physical action amid young people: the AIMFIT pragmatic randomized controlled trial. JMIR. 2015;17:e210.
-
Hebden L, Cook A, van der Ploeg HP, King L, Bauman A, Allman-Farinelli Yard. A mobile health intervention for weight management among young adults: a pilot randomised controlled trial. J Hum Nutr Diet. 2014;27:322–32.
-
Kirwan Yard, Duncan MJ, Vandelanotte C, Mummery WK. Using smartphone engineering to monitor physical activity in the 10,000 Steps program: a matched instance-control trial. JMIR. 2012;xiv:e55.
-
Maher C, Ferguson M, Vandelanotte C, Plotnikoff R, De Bourdeaudhuij I, Thomas Southward, et al. A web-based, social networking physical action intervention for insufficiently agile adults delivered via facebook app: randomised controlled trial. JMIR. 2015;17:e174.
-
Gilson ND, Pavey TG, Vandelanotte C, Duncan MJ, Gomersall SR, Trost SG, et al. Chronic disease risks and utilise of a smartphone awarding during a physical activity and dietary intervention in Australian truck drivers. Aust N Z J Public Health. 2016;forty:91–3.
-
Gasser R, Brodbeck D, Degen Grand, Luthiger J, Wyss R, Reichlinal S. Persuasiveness of a mobile lifestyle coaching application using social facilitation. Pers Technol. 2006;3962:27–38.
-
Glynn LG, Hayes PS, Casey M, Glynn F, Alvarez-Iglesias A, Newell J, et al. Effectiveness of a smartphone application to promote physical activity in main intendance: the SMART MOVE randomised controlled trial. Br J Gen Pract. 2014;64:e384–91.
-
van Drongelen A, Boot CRL, Hlobil H, Twisk JWR, Smid T, van der Beek AJ. Evaluation of an mHealth intervention aiming to meliorate health-related behavior and sleep and reduce fatigue among airline pilots. Scand J Piece of work Environ Wellness. 2014;twoscore:557–68.
-
Walsh JC, Corbett T, Hogan M, Duggan J, McNamara A. An mHealth intervention using a smartphone app to increase walking behavior in young adults: a pilot study. JMIR Mhealth Uhealth. 2016;4:e109.
-
Rospo G, Valsecchi V, Bonomi AG, Thomassen IWG, van Dantzig S, La Torre A, et al. Cardiorespiratory improvements achieved by American College of sports medicine's practice prescription implemented on a mobile app. JMIR Mhealth Uhealth. 2016;4:e77.
-
Elbert SP, Dijkstra A, Oenema A. A mobile phone app intervention targeting fruit and vegetable consumption: the efficacy of textual and auditory tailored health information tested in a randomized controlled trial. J Med Internet Res. 2016;18:e147.
-
Safran Naimark J, Madar Z, Shahar DR. The impact of a web-based app (eBalance) in promoting healthy lifestyles: randomised controlled trial. JMIR. 2015;17:e56.
-
Flecha OD, de Oliveira DWD, Marques LS, Gonçalves PF. A commentary on randomized clinical trials: How to produce them with a good level of bear witness. Perspect Clin Res. 2016;7:75–80.
-
Dennison 50, Morrison 50, Conway Thou, Yardley 50. Opportunities and challenges for smartphone applications in supporting wellness behavior modify: qualitative study. JMIR. 2013;xv:e86.
-
Guertler D, Vandelanotte C, Kirwan M, Duncan MJ. Engagement and nonusage attrition with a costless physical activeness promotion program: the instance of ten,000 steps Australia. JMIR. 2015;17:e176.
-
Nikoloudakis IA, Vandelanotte C, Rebar AL, Schoeppe S, Aisle S, Duncan MJ, et al. Examining the correlates of online health information-seeking behavior among men compared with women. Am J Mens Wellness. 2016; 2016. doi:10.1177/1557988316650625.
-
De Bourdeaudhuij I, Van Cauwenberghe E, Spittaels H, Oppert JM, Rostami C, Brug J, et al. School-based interventions promoting both physical activity and healthy eating in Europe: a systematic review inside the Promise project. Obes Rev. 2011;12:205–xvi.
-
Kriemler South, Meyer U, Martin E, Van Sluijs EMF, Andersen LB, Martin BW. Event of school-based interventions on physical activity and fitness in children and adolescents: a review of reviews and systematic update. Br J Sports Med. 2011;45:923–30.
-
Rodrigues AL, Ball J, Ski C, Stewart Southward, Carrington MJ. A systematic review and meta-analysis of principal prevention programmes to meliorate cardio-metabolic take a chance in non-urban communities. Prev Med. 2016;87:22–34.
-
Appleton KM, Hemingway A, Saulais 50, Dinnella C, Monteleone Eastward, Depezay L, et al. Increasing vegetable intakes: rationale and systematic review of published interventions. Eur J Nutr. 2016;2016(55):869–96.
-
Greaves CJ, Sheppard KE, Abraham C, Hardeman Westward, Roden Grand, Evans PH, et al. Systematic review of reviews of intervention components associated with increased effectiveness in dietary and physical activeness interventions. BMC Public Health. 2011;eleven:119.
-
Vandelanotte C, Spathonis KM, Eakin EG, Owen North. Website-delivered physical activity interventions. A review of the literature. Am J Prev Med. 2007;33:54–64.
-
O'Reilly GA, Spruijt-Metz D. Current mHealth technologies for physical activity assessment and promotion. Am J Prev Med. 2013;45:501–7.
-
Pew Research Center. Teens, social media & technology overview 2015: smartphones facilitate shifts in communication mural for teens. Pew Research Middle. 2015. http://www.pewinternet.org/files/2015/04/PI_TeensandTech_Update2015_0409151.pdf. Accessed v Jul 2016.
-
Boulos MNK, Yang SP. Exergames for health and fitness: the roles of GPS and geosocial apps. Int J Health Geogr. 2013;12:18.
-
Neve M, Morgan PJ, Jones PR, Collins CE. Effectiveness of spider web-based interventions in achieving weight loss and weight loss maintenance in overweight and obese adults: a systematic review with meta-analysis. Obes Rev. 2010;11:306–21.
-
Dumville JC, Torgerson DJ, Hewitt CE. Reporting attrition in randomised controlled trials. BMJ. 2006;332:969–71.
-
van Genugten L, Dusseldorp E, Webb T, van Empelen P. Which combinations of techniques and modes of delivery in internet-based interventions effectively change health beliefs? A meta-analysis. JMIR. 2016;18:e155.
-
Middelweerd A, van der Laan DM, van Stralen MM, Mollee JS, Stuij M, te Velde SJ, et al. What features do Dutch university students prefer in a smartphone application for promotion of concrete activity? A qualitative approach. Int J Behav Nutr Phys Act. 2015;12:31.
-
Webb TL, Joseph J, Yardley 50, Michie S. Using the internet to promote wellness behavior modify: a systematic review and meta-analysis of the bear upon of theoretical basis, use of behavior change techniques, and mode of delivery on efficacy. JMIR. 2010;12:e4.
-
Sandholzer Chiliad, Deutsch T, Frese T, Winter A. Predictors of students' cocky-reported adoption of a smartphone application for medical education in full general practice. BMC Med Educ. 2015;fifteen:91.
-
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JP, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ. 2009;339:b2700.
Acknowledgements
SS is supported by an Early Career Fellowship (GNT1125586) from the Australian National Health and Medical Research Quango. CV (ID 100427) and MJD (ID 100029) are supported by Futurity Leader Fellowships from the National Centre Foundation of Australia.
Funding
SS is supported past an Early Career Fellowship (GNT1125586) from the Australian National Health and Medical Research Council. CV (ID 100427) and MJD (ID 100029) are supported by Time to come Leader Fellowships from the National Heart Foundation of Australia.
Availability of data and materials
Not applicable.
Authors' contributions
SS, SA, WVL and CV conceptualised and designed the study. SS, SA, WVL and NAB conducted the search, article selection, data extraction and quality assessment. SS drafted and wrote the manuscript. SA, WVL, CV, MJD, SLW, and NAB were involved in estimation of information and critically revising the manuscript. All authors read and approved the last manuscript.
Competing interests
The authors declare that they have no competing interests.
Consent for publication
Not applicable.
Ethics blessing and consent to participate
Not applicable.
Author information
Affiliations
Respective author
Additional files
Rights and permissions
Open Admission This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/past/iv.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided yous give appropriate credit to the original author(s) and the source, provide a link to the Artistic Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data fabricated bachelor in this commodity, unless otherwise stated.
Reprints and Permissions
About this commodity
Cite this article
Schoeppe, South., Alley, S., Van Lippevelde, Due west. et al. Efficacy of interventions that utilize apps to improve nutrition, concrete action and sedentary behaviour: a systematic review. Int J Behav Nutr Phys Act thirteen, 127 (2016). https://doi.org/10.1186/s12966-016-0454-y
-
Received:
-
Accepted:
-
Published:
-
DOI : https://doi.org/ten.1186/s12966-016-0454-y
Keywords
- Systematic review
- Literature searches
- Smartphone applications
- Programs
- Efficacy
- Healthy eating
- Exercise
- Sitting
- Health behaviour
Source: https://ijbnpa.biomedcentral.com/articles/10.1186/s12966-016-0454-y
0 Response to "Mobile Phone Interventions to Increase Physical Activity and Reduce Weight a Systematic Review"
Post a Comment